Role of fecal microbiota transplantation in treating slow transit constipation based on 16S rDNA detection
-
摘要:目的
通过16S rDNA检测技术探讨慢传输型便秘(STC)患者肠道菌群特点以及肠道菌群移植(FMT)的作用。
方法选取30例STC患者作为STC组,给予2个疗程的规范化FMT治疗; 选取同期20例健康成年人作为对照组。采用粪便16S rDNA测序技术对STC组和对照组肠道菌群进行比较,并对STC患者实施FMT前后的肠道菌群进行比较。
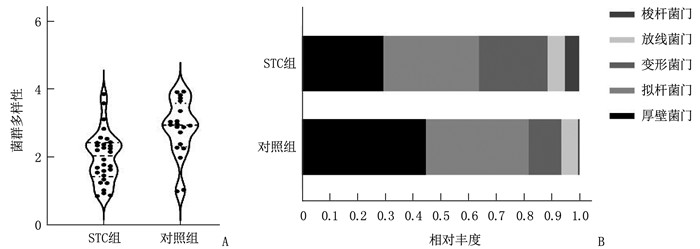
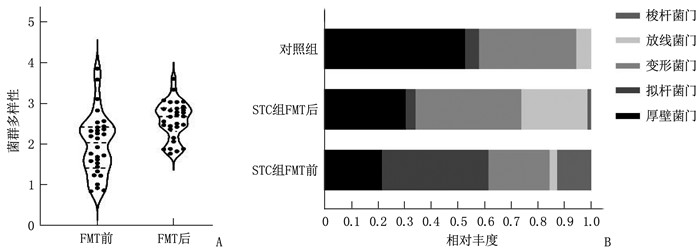
结果与对照组相比, STC组肠道菌群多样性降低,厚壁菌门相对丰度降低,而变形菌门和梭杆菌门相对丰度升高,差异均有统计学意义(P < 0.05)。经FMT治疗后,功能性便秘患者菌群多样性升高,差异有统计学意义(P < 0.05); 在门水平上, STC患者实施FMT后拟杆菌门和梭状菌门相对丰度降低,而厚壁菌门和变形菌门相对丰度升高,差异有统计学意义(P < 0.05)。STC组胃肠生活质量评分(GIQLI)、Wexner便秘评分均较治疗前下降,差异有统计学意义(P < 0.05)。STC组抑郁自评量表(SDS)评分、焦虑自评量表(SAS)评分、匹兹堡睡眠质量评分(PSQI)均较治疗前下降,差异有统计学意义(P < 0.05)。
结论STC患者肠道菌群易发生紊乱,菌群多样性及分布发生改变。FMT可通过调节肠道菌群来改善便秘症状,改变肠道菌群的分布和多样性。
-
关键词:
- 慢传输型便秘 /
- 肠道菌群 /
- 肠道菌群移植 /
- 16S rDNA检测技术
Abstract:ObjectiveTo investigate the characteristics of intestinal flora in patients with slow transit constipation (STC) and role of fecal microbiota transplantation (FMT) by 16S rDNA sequencing technology.
MethodsA total of 30 patients with STC were selected as STC group, and they were treated with standardized FMT therapy for two courses; another 20 healthy adults in the same period were selected as control group. Fecal 16S rDNA sequencing technology was used to compare the intestinal flora between the control group and the STC group, and the intestinal flora before and after FMT in patients with STC was compared.
ResultsCompared with the control group, the diversity of intestinal flora in the STC group decreased significantly, the relative abundance of Firmicutes decreased significantly, and the relative abundances of Proteobacteria and Fusobacteria increased significantly (P < 0.05). After FMT treatment, the diversity of flora in patients with functional constipation increased significantly (P < 0.05); at the phylum level, the relative abundances of Bacteroidetes and Fusobacteria decreased significantly while the relative abundances of Firmicutes and Proteobacteria increased significantly in STC patients after implementing FMT (P < 0.05). The Gastrointestinal Quality of Life Index (GIQLI) score and Wexner constipation score in the STC group decreased significantly after treatment when compared to those before treatment (P < 0.05). The Self-rating Depression Scale (SDS) score, Self-rating Anxiety Scale (SAS) score and Pittsburgh Sleep Quality Index (PSQI) score in the STC group decreased significantly after treatment when compared to those before treatment (P < 0.05).
ConclusionSTC patients are prone to disruption of intestinal flora, resulting in changes of microbial diversity and distribution. FMT can improve constipation symptoms and change the distribution and diversity of intestinal flora by regulating intestinal flora.
-
-
表 1 STC组和对照组粪便菌群比较(x ± s[M(IQR)]
组别 菌群多样性 厚壁菌门 拟杆菌门 变形菌门 放线菌门 梭杆菌门 STC组 2.00±0.76 0.29±0.24 0.34±0.25 0.25±0.20 0.03(0.01~0.05) 0.01(0~0.07) 对照组 2.84±0.84* 0.45±0.21* 0.37±0.28 0.12±0.11* 0.05(0.01~0.07) 0.02(0~0.01)* 与STC组比较, *P<0.05。 表 2 STC患者FMT前后粪便菌群比较(x ± s)[M(IQR)]
时点 菌群多样性 厚壁菌门 拟杆菌门 变形菌门 放线菌门 梭杆菌门 FMT前 2.00±0.76 0.29±0.24 0.34±0.25 0.25±0.20 0.03(0.01~0.05) 0.01(0~0.07) FMT后 2.60±0.47* 0.47±0.11* 0.10±0.10* 0.33±0.16* 0.04(0.01~0.09) 0(0~0.02)* 与FMT前比较, *P<0.05。 表 3 STC患者实施FMT前后精神心理评估及疗效评估(x ± s)
分 时点 SDS评分 SAS评分 PSQI GIQLI Wexner便秘评分 FMT前 44.73±9.18 44.50±7.62 10.03±3.98 66.63±16.36 15.17±1.49 FMT后 39.03±8.20* 35.77±7.47* 8.23±2.70* 50.40±16.13* 2.27±1.14* SDS: 抑郁自评量表; SAS: 焦虑自评量表; PSQI: 匹兹堡睡眠质量评分; GIQLI: 胃肠生活质量指数。与FMT前比较, *P<0.05。 表 4 STC患者实施FMT前后BMI和血检指标比较(x ± s)
时点 BMI/(kg/m2) RBC/(×1012/L) WBC/(×109/L) ALT/(U/L) AST/(U/L) CREA/(μmol/L) UREA/(mmol/L) FMT前 22.27±2.08 4.12±0.62 4.27±0.68 16.14±6.14 30.03±8.88 66.97±10.45 4.70±1.19 FMT后 22.30±2.02 4.14±0.55 4.29±0.51 14.57±4.17 28.03±5.88 66.67±9.85 4.49±0.93 -
[1] TAMURA A, TOMITA T, OSHIMA T, et al. Prevalence and self-recognition of chronic constipation: results of an Internet survey[J]. J Neurogastroenterol Motil, 2016, 22(4): 677-685.
[2] LONG Y, HUANG Z, DENG Y, et al. Prevalence and risk factors for functional bowel disorders in South China: a population based study using the Rome Ⅲ criteria[J]. Neurogastroenterol Motil, 2017, 29(1): 1-9.
[3] 中华医学会消化病学分会胃肠动力学组, 中华医学会消化病学分会功能性胃肠病协作组. 中国慢性便秘专家共识意见(2019, 广州)[J]. 中华消化杂志, 2019, 39(9): 577-598. doi: 10.3760/cma.j.issn.0254-1432.2019.09.001 [4] HUANG L S, ZHU Q, QU X, et al. Microbial treatment in chronic constipation[J]. Sci China Life Sci, 2018, 61(7): 744-752. doi: 10.1007/s11427-017-9220-7
[5] KELLY C R, KAHN S, KASHYAP P, et al. Update on fecal microbiota transplantation 2015: indications, methodologies, mechanisms, and outlook[J]. Gastroenterology, 2015, 149(1): 223-237. doi: 10.1053/j.gastro.2015.05.008
[6] 张发明, 龙楚彦, 李潘. 粪菌移植体系的整体整合医学思考[J]. 生命科学, 2017, 29(7): 651-659. doi: 10.13376/j.cbls/2017089 [7] BRUMBAUGH D E, DE ZOETEN E F, PYO-TWIST A, et al. An Intragastric Fecal Microbiota Transplantation Program for Treatment of Recurrent Clostridium difficile in Children is Efficacious, Safe, and Inexpensive[J]. J Pediatr, 2018, 194: 123-127, e1. doi: 10.1016/j.jpeds.2017.10.016
[8] ZHAO Y, YU Y B. Intestinal microbiota and chronic constipation[J]. SpringerPlus, 2016, 5(1): 1130. doi: 10.1186/s40064-016-2821-1
[9] WANG Y F, DONG Q B, HU S X, et al. Decoding microbial genomes to understand their functional roles in human complex diseases[J]. iMeta, 2022, 1(2): e14.
[10] WEI Y J, LI X Q, JI B Y, et al. Recent advances on the recovery, modulation and synthetic biology of gut microbiota and hosts[J]. Sci Sin-Vitae, 2022, 52(2): 249-265. doi: 10.1360/SSV-2021-0088
[11] 中华医学会肠外肠内营养学分会, 中国国际医疗保健促进交流会加速康复外科分会, 中国微生态治疗创新联盟, 等. 菌群移植标准化方法学的建立与临床应用中国专家共识[J]. 中华胃肠外科杂志, 2020, 23(S1): 5-13. [12] SENDER R, FUCHS S, MILO R. Are we really vastly outnumbered revisiting the ratio of bacterial to host cells in humans[J]. Cell, 2016, 164(3): 337-340. doi: 10.1016/j.cell.2016.01.013
[13] ROBERTSON S J, GOETHEL A, GIRARDIN S E, et al. Innate immune influences on the gut microbiome: lessons from mouse models[J]. Trends Immunol, 2018, 39(12): 992-1004. doi: 10.1016/j.it.2018.10.004
[14] HILL J H, ROUND J L. SnapShot: Microbiota effects on host physiology[J]. Cell, 2021, 184(10): 2796-2796, e1. doi: 10.1016/j.cell.2021.04.026
[15] AARNOUTSE R, ZIEMONS J, PENDERS J, et al. The clinical link between human intestinal microbiota and systemic cancer therapy[J]. Int J Mol Sci, 2019, 20(17): 4145. doi: 10.3390/ijms20174145
[16] 张成岗, 巩文静, 李志慧, 等. 双脑模型假说—由肠道菌群微生态构建的"菌脑"可能是人体对物质记忆的"第二大脑"[J]. 实用临床医药杂志, 2019, 23(6): 1-6. doi: 10.7619/jcmp.201906001 [17] LI Q, GUO L, WANG L, et al. Composition of "Gold Juice" Using an Ancient Method Based on Intestinal Microecology[J]. The Journal of International Medical Research, 2020, 48(9): 1-18.
[18] LIU T H, YANG Z S, ZHANG X M, et al. 16S rDNA analysis of the effect of fecal microbiota transplantation on pulmonary and intestinal flora[J]. 3 Biotech, 2017, 7(6): 370. doi: 10.1007/s13205-017-0997-x
[19] 刘昌孝. 肠道菌群与健康、疾病和药物作用的影响[J]. 中国抗生素杂志, 2018, 43(1): 1-14. doi: 10.3969/j.issn.1001-8689.2018.01.001 [20] 国家卫生健康委员会医院管理研究所, 中华医学会肠外肠内营养学分会, 中华医学会肠外肠内营养学分会肠道微生态协作组. 肠道菌群移植临床应用管理中国专家共识(2022版)[J]. 中华胃肠外科杂志, 2022, 25(9): 747-756. doi: 10.3760/cma.j.cn441530-20220725-00324 [21] 陈启仪, 杨波, 田宏亮, 等. 菌群移植3 932例治疗效果和并发症的5年随访分析[J]. 中华消化杂志, 2020, 40(11): 768-777. [22] 赵琪, 房永坤, 严成, 等. 经自然腔道取标本手术联合金陵术治疗顽固性便秘的疗效分析[J]. 实用临床医药杂志, 2022, 26(12): 69-75. doi: 10.7619/jcmp.20220092 [23] 刘启鸿, 方文怡, 胡露楠, 等. 基于16S rRNA高通量测序技术分析福州地区慢传输型便秘患者肠道菌群的变化[J]. 中国微生态学杂志, 2022, 34(3): 323-326. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGWS202203015.htm [24] 徐蓓蓓, 黄益, 叶毅, 等. 慢传输型便秘患者肠黏膜菌的变化特征[J]. 中国药物与临床, 2019, 19(24): 4293-4296. https://www.cnki.com.cn/Article/CJFDTOTAL-YWLC201924031.htm [25] GUO M Q, YAO J F, YANG F, et al. The composition of intestinal microbiota and its association with functional constipation of the elderly patients[J]. Future Microbiol, 2020, 15: 163-175. doi: 10.2217/fmb-2019-0283
[26] CHEN Y T, WU T, LU W W, et al. Predicting the role of the human gut microbiome in constipation using machine-learning methods: a meta-analysis[J]. Microorganisms, 2021, 9(10): 2149. doi: 10.3390/microorganisms9102149
[27] 徐岚, 谢忱, 殷民月, 等. 功能性便秘临床症状与肛门直肠测压特征的相关性研究[J]. 实用临床医药杂志, 2023, 27(2): 67-72. doi: 10.7619/jcmp.20221852 [28] 刘巍, 刘晓红, 方秀才, 等. 北京地区门诊慢性便秘患者多中心流行病学调查[J]. 胃肠病学, 2010, 15(2): 95-98. https://www.cnki.com.cn/Article/CJFDTOTAL-WIEC201002010.htm [29] CHEN L M, WANG D M, GARMAEVA S, et al. The long-term genetic stability and individual specificity of the human gut microbiome[J]. Cell, 2021, 184(9): 2302-2315. e12.
[30] 叶雅玲, 钱希, 吕璨. 睡眠障碍对老年慢性功能性便秘患者焦虑抑郁情绪和生活质量的影响分析[J]. 世界华人消化杂志, 2020, 28(11): 443-447. https://www.cnki.com.cn/Article/CJFDTOTAL-XXHB202011011.htm [31] MIYAOKA T, KANAYAMA M, WAKE R, et al. Clostridium butyricum MIYAIRI 588 as adjunctive therapy for treatment-resistant major depressive disorder: a prospective open-label trial[J]. Clin Neuropharmacol, 2018, 41(5): 151-155.
-
期刊类型引用(4)
1. 吴蓓,郭辉,卢沛,陈景,王聪,郭倩倩,余海波. 授权理论的护理模式对胆囊切除术后患者自我护理能力及心理状态影响. 中国健康心理学杂志. 2025(02): 253-257 .  百度学术
百度学术
2. 代立群,王静,胡毛姐. 阶段性功能锻炼联合回馈式健康宣教对出血性脑卒中后偏瘫患者的干预效果. 实用心脑肺血管病杂志. 2025(04): 64-68+74 .  百度学术
百度学术
3. 戴玲,周建伟,郑明香,彭兰芳. 基于社会认知理论的冠心病经皮冠状动脉介入术后Ⅱ期远程家庭心脏康复方案的构建. 实用临床医药杂志. 2024(22): 110-114 .  本站查看
本站查看
4. 陈志琴. 医养结合理念指导下的中医护理模式在冠心病PCI后康复中的应用. 心血管病防治知识. 2024(18): 81-84 .  百度学术
百度学术
其他类型引用(0)




 下载:
下载:
 苏公网安备 32100302010246号
苏公网安备 32100302010246号